Dr.A.Deepak Thirunavukkarasu MBBS, DDVL, Fellow in Medical Cosmetology
Eczema Treatment in Chennai
Call Us
+91 7200148548
Email Us
cutikidz2022@gmail.com
Book Your appointment
Why Choose CutiKidz Skin Clinic for Eczema Treatment in Chennai ?
Choose CutiKidz Skin Clinic for Eczema Treatment in Chennai for Expert Care and Effective Solutions. Our Dermatologists Specialize in Personalized Treatment Plans Tailored to Your Child’s Needs, Ensuring Comfort and Relief. Book Your Appointment Today for Professional Eczema Management and Improved Skin Health
Expert Dermatologists: At CutiKidz, your child’s skin health is in the hands of experienced dermatologists who specialize in pediatric dermatology. Our team understands the nuances of childhood eczema and employs evidence-based approaches for effective management.
Personalized Treatment Plans: We recognize that every child’s eczema is different. That’s why we take a personalized approach to treatment, tailoring our strategies to suit your child’s specific condition, triggers, and lifestyle. This ensures the most effective and comfortable treatment experience.
Comprehensive Care: Our clinic offers comprehensive care for eczema, addressing not only the symptoms but also the underlying causes and triggers. From thorough evaluations to ongoing management and support, we’re committed to providing holistic care for your child’s skin health.
Child-Friendly Environment: We understand that visiting the doctor can be intimidating for children. That’s why our clinic is designed to be warm, welcoming, and child-friendly. Our compassionate staff and relaxed atmosphere help create a positive experience for your child, making treatment visits stress-free.
Cutting-Edge Treatments: CutiKidz Skin Clinic stays abreast of the latest advancements in eczema treatment. We offer a range of cutting-edge therapies, including topical treatments, phototherapy, and emerging biologic therapies, ensuring that your child has access to the most innovative and effective treatment options available.
Education and Support: We believe in empowering parents and children with the knowledge and tools they need to manage eczema effectively. Our team provides education on eczema triggers, skincare routines, and lifestyle modifications to help prevent flare-ups and promote long-term skin health.
Proven Results: Our track record speaks for itself. CutiKidz Skin Clinic has helped numerous children successfully manage their eczema, leading to improved skin health, reduced symptoms, and enhanced quality of life.
When you choose CutiKidz Skin Clinic for eczema treatment in Chennai, you’re choosing expert care, personalized attention, and a commitment to your child’s skin health and well-being. Book an appointment with us today and take the first step towards relieving your child’s eczema symptoms and restoring their confidence in their skin
What is eczema?
Eczema, also known as dermatitis, is a chronic inflammatory skin condition characterized by patches of dry, itchy, red, and inflamed skin. It can occur at any age but is more common in infants and children. Eczema is believed to be caused by a combination of genetic, environmental, and immune system factors.
Solutions for Eczema

Wet Wrap Therapy
This involves applying a moisturizer or topical medication to the skin, followed by wrapping the affected area with damp bandages or clothing. Wet wrap therapy helps to soothe the skin, reduce inflammation
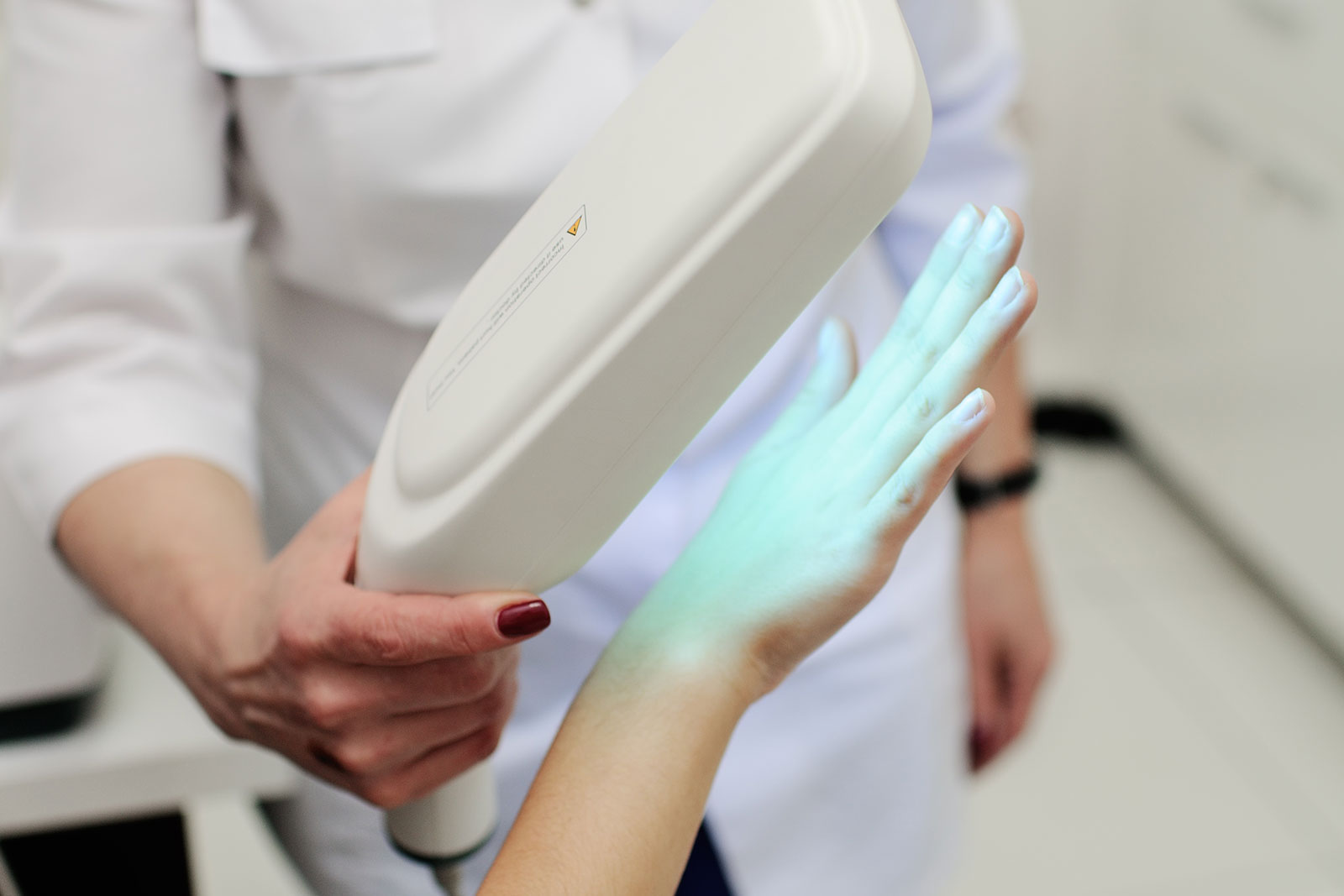
Phototherapy (Light Therapy)
Controlled exposure to ultraviolet (UV) light under medical supervision can help reduce inflammation, itching, and the severity of eczema symptoms.
Medications Practice
Using some drugs alone or in combination with other therapies can restore some of the skin tones
Symptoms of eczema
Dry, Itchy Skin: Eczema often causes dryness and itching, which can be intense and persistent. The itching can worsen at night, leading to sleep disturbances.
Redness: Affected areas of the skin may appear red or inflamed, especially during flare-ups or when the skin is irritated.
Rashes: Eczema can cause rashes that may be red, patchy, or raised. These rashes can occur anywhere on the body but are commonly found on the face, neck, hands, elbows, and behind the knees.
Skin Swelling: Inflammation associated with eczema can lead to swelling of the affected skin, making it appear puffy or swollen.
Cracking and Flaking: Dry, irritated skin can crack and peel, leading to flaking or scaling. This can result in rough or scaly patches of skin.
Blisters or Oozing: In some cases, eczema may cause small fluid-filled blisters that can rupture and ooze clear fluid. This is more common in severe cases or during acute flare-ups.
Thickened Skin: Chronic scratching or rubbing of the affected skin can lead to thickening and hardening of the skin, known as lichenification. This can make the skin feel rough and leathery.
Sensitive Skin: People with eczema often have sensitive skin that may react strongly to certain triggers, such as harsh soaps, detergents, or environmental allergens.
Secondary Infections: Constant scratching can break the skin barrier, making it susceptible to bacterial or fungal infections. Signs of infection include increased redness, swelling, warmth, pain, and pus-filled lesions.
Emotional Distress: Living with eczema can take a toll on a person’s emotional well-being, leading to feelings of frustration, embarrassment, anxiety, or depression, especially if the condition is severe or persistent.
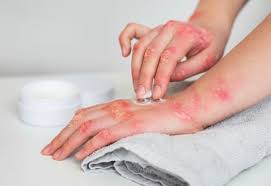
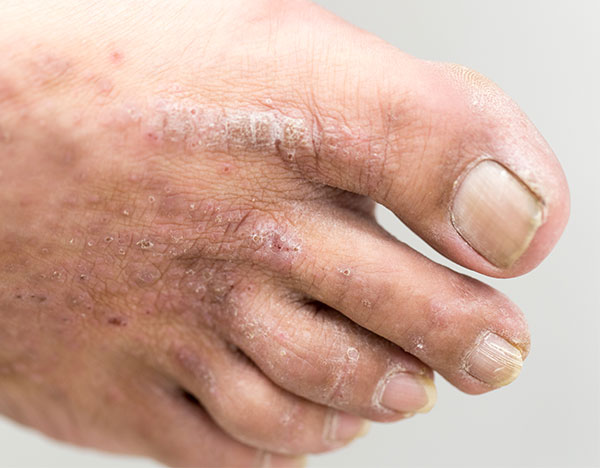
Types of Eczema
Eczema, or atopic dermatitis, can manifest in different types, each with its own characteristics and affected areas of the body. The main types of eczema include:
- Atopic Dermatitis: This is the most common type of eczema and often appears in infancy or early childhood. It is characterized by red, itchy rashes on the face, scalp, elbows, knees, and other areas of the body. Atopic dermatitis is associated with a family history of allergic conditions like asthma or hay fever.
Contact Dermatitis: Contact dermatitis occurs when the skin comes into direct contact with an irritant or allergen, leading to inflammation and irritation. There are two types of contact dermatitis:
- Irritant Contact Dermatitis: Caused by exposure to substances like harsh chemicals, soaps, or detergents.
- Allergic Contact Dermatitis: Triggered by an allergic reaction to specific substances like metals (e.g., nickel), latex, or certain cosmetics.
Dyshidrotic Eczema: Also known as pompholyx eczema, this type primarily affects the hands and feet. It is characterized by small, fluid-filled blisters that itch and may be accompanied by redness and scaling. Episodes of dyshidrotic eczema may be triggered by stress, exposure to certain metals, or environmental factors.
Nummular Eczema: Nummular eczema presents as coin-shaped patches of irritated, inflamed skin that may ooze or crust over. These patches are typically found on the arms, legs, back, or buttocks and can be intensely itchy. Nummular eczema is more common in older adults and may be triggered by dry skin, injury, or allergens.
Seborrheic Dermatitis: While not strictly categorized as eczema, seborrheic dermatitis shares similar characteristics and may be considered a type of eczema. It affects areas of the body with a high density of oil glands, such as the scalp, face, and chest. Symptoms include redness, greasy or scaly patches, and itching. Seborrheic dermatitis is associated with an overgrowth of yeast on the skin and may worsen with stress or hormonal changes.
What can I do at home?
- Oatmeal Baths: Adding colloidal oatmeal to bathwater can soothe irritated skin and relieve itching. Oatmeal contains compounds that have anti-inflammatory properties and help moisturize the skin.
- Coconut Oil: Applying virgin coconut oil to eczema-affected areas can help moisturize the skin and reduce inflammation. Coconut oil contains fatty acids that help strengthen the skin barrier and prevent moisture loss.
- Aloe Vera Gel: Aloe vera has soothing and anti-inflammatory properties that can help reduce redness and irritation associated with eczema. Applying fresh aloe vera gel to the affected skin may provide relief.
- Cold Compresses: Applying cold compresses or ice packs to eczema-affected areas can help alleviate itching and reduce inflammation. Wrap the ice pack in a thin cloth to prevent skin damage from direct contact.
- Apple Cider Vinegar: Diluted apple cider vinegar can help restore the skin’s natural pH balance and relieve itching. Mix equal parts of apple cider vinegar and water and apply it to the affected areas with a cotton ball. Be sure to dilute it well to avoid skin irritation.
- Honey: Applying raw honey to eczema patches may help soothe the skin and reduce inflammation. Honey has antimicrobial properties that can help prevent infections and promote healing.
- Probiotics: Consuming probiotic-rich foods or taking probiotic supplements may help improve gut health and reduce inflammation, which can benefit eczema symptoms.
- Wet Wraps: After applying moisturizer or a mild corticosteroid cream to the affected areas, cover them with damp gauze or clothing and then a dry layer to lock in moisture and enhance the effectiveness of topical treatments.
- Avoiding Triggers: Identify and avoid triggers that exacerbate eczema symptoms, such as harsh soaps, fragrances, certain fabrics, and environmental allergens.
- Stress Management: Practicing stress-reduction techniques such as mindfulness, meditation, yoga, or deep breathing exercises may help reduce eczema flare-ups triggered by stress.
Causes of eczema
The exact cause of eczema, also known as atopic dermatitis, is not fully understood, but it is believed to involve a combination of genetic, environmental, and immune system factors. Common causes and contributing factors to eczema include:
Genetic Predisposition: Individuals with a family history of eczema, asthma, hay fever (allergic rhinitis), or other allergic diseases are more likely to develop eczema. Certain genetic variations can affect the skin’s barrier function and immune response, increasing susceptibility to eczema.
Immune System Dysfunction: Eczema is associated with abnormalities in the immune system, including an overactive immune response and increased levels of inflammation in the skin. This immune dysregulation can lead to chronic inflammation and skin barrier dysfunction characteristic of eczema.
Skin Barrier Dysfunction: Eczema is characterized by a defective skin barrier, which allows moisture to escape and irritants, allergens, and microbes to penetrate the skin more easily. Factors contributing to skin barrier dysfunction include:
- Deficiency of filaggrin protein, which plays a crucial role in maintaining the skin barrier.
- Disruption of lipid (fat) composition in the skin, impairing its ability to retain moisture.
- Damage from scratching, friction, or exposure to harsh chemicals or irritants.
Environmental Triggers: Exposure to certain environmental factors can exacerbate eczema symptoms or trigger flare-ups. Common environmental triggers include:
- Allergens: Dust mites, pollen, pet dander, mold, and certain foods.
- Irritants: Harsh soaps, detergents, cleaning products, fragrances, and wool clothing.
- Climate: Dry or cold weather, low humidity, and exposure to extreme temperatures.
- Microbes: Bacteria, viruses, and fungi that can colonize and infect eczema-prone skin.
Hormonal Changes: Hormonal fluctuations, particularly during puberty or pregnancy, can influence eczema symptoms. Changes in hormone levels may affect skin hydration, inflammation, and immune response, potentially exacerbating eczema.
Stress and Emotional Factors: Psychological stress, anxiety, and emotional factors can exacerbate eczema symptoms or trigger flare-ups through mechanisms involving the immune system and neuroendocrine pathways.
